Study reveals potential new way to burn fat faster
Post Date: May 18, 2021 | Publish Date: May 18, 2021
Multi-center team led by scientists at Cincinnati Children’s reports finding a ‘good’ form of inflammation that allows mice to avoid obesity
Over the years, research has shown that obesity and the immune system can reciprocally play havoc with human health. But in a new study, scientists have detected one set of inflammatory mediators that appears to prevent weight gain rather than aggravate the consequences of obesity.
Detailed findings were published online May 18, 2021, in Nature Communications.
“Typically, obesity induces a chronic, low-level state of inflammation that increases a person’s risk of developing diabetes, cardiovascular disease and non-alcoholic fatty liver disease (NAFLD),” says Senad Divanovic, PhD, a member of the Division of Immunobiology at Cincinnati Children’s and corresponding author for the study. “But our novel findings indicate that increasing activity along one particular axis of inflammation actually prevents weight gain in mice given obesity-inducing diets.”
BAFF/APRIL axis plays unexpected role in weight control
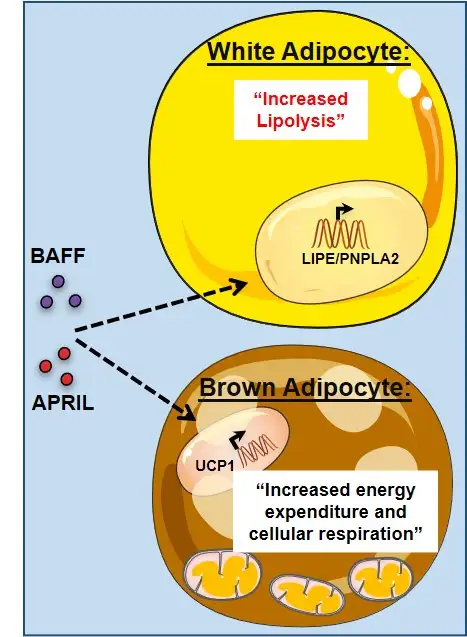
That axis involves two closely related proteins called BAFF and APRIL. Both are known to researchers for their role in regulating B-cell activity in the immune system. But until now, they were not known to play a major role in obesity.
Mice that produced high levels of these proteins kept their weight in check, even when fed diets that normally cause obesity. Mice bred to utterly lack these proteins gained weight at a rapid pace.
This study was the first to highlight how these proteins drive a multi-faceted mechanism on different types of fat. One mechanism was observed to cause white fat, the tissue which in excess leads to obesity, to break down into its original building blocks. The other mechanism instructed the body’s brown fat, a specialized type of body fat that burns energy to warm the body, to turn on.
The findings suggest that rebalancing the BAFF/APRIL pathway in obese people might help prevent weight gain. The team found that the BAFF/APRIL activity on white fat seen in mice also occurs in humans. In fact, the team noted that people lost more weight after receiving bariatric surgery if they also had higher levels of BAFF/APRIL.
Next steps
In mice, the researchers used gene editing to control expression of the BAFF and APRIL proteins. While drugs already exist that can inhibit BAFF’s function, scientists need to discover a drug compound that can augment BAFF and APRIL protein levels. Further, careful studies to comprehend how such compounds can turn on BAFF and APRIL’s effects selectively in white and brown fat would be significant.
That work is just beginning, Divanovic says. Further study also is needed to make sure that controlling BAFF/APRIL levels to prevent obesity does not lead to unwanted problems with altered B-cell function.
So, while the study provides a potentially exciting new approach, it will likely be several years before this discovery could lead to a practical anti-obesity treatment, Divanovic says. However, new findings presented in this research could be used as predictive tools to identify people who may benefit the most from bariatric surgery and the subsequent weight loss.
About this study
In addition to Divanovic, co-authors from Cincinnati Children’s and the University of Cincinnati include Calvin Chan (lead author), Isaac Harley (co-lead author), Aurelien Trompette, Traci Stankiewicz, Jessica Allen, Maria Moreno-Fernandez, Michelle Damen, Jarren Oates, Pablo Alarcon, Jessica Doll, Matthew Flick, Leah Flick, Joan Sanchez-Gurmaches, Rajib Mukherjee, Rebekah Karns, and Michael Helmrath.
Co-authors also include experts from Children’s Hospital Colorado; Columbia University Medical Center; the Helmholtz Center, the German Center for Diabetes Research and the Technische Universitat in Germany; Stanford University; the Veterans Affairs Palo Alto Health Care System; and the Bill & Melinda Gates Foundation.
This study was supported, in part, by grants from the American Diabetes Association (1-18-IBS-100, 1-19-PMF-019); the National Institutes of Health (R01DK099222, R21AI139829, R01AI075159, T32AI118697, T32GM063483-14, HD07463 and GM063483); the U.S. Department of Defense (W81XWH2010392); American Heart Association (17POST33650045, 18CDA34080527, 19POST34380545); the Albert J. Ryan Foundation Fellowship; PHS Grant P30 DK078392; the Pediatric Diabetes and Obesity Center, the Digestive Disease Research Core Center and a Trustee Award from Cincinnati Children’s; the Marie Skłodowska Curie training network “ChroMe” grant; the German Center for Diabetes Research; and support from the Helmholtz Association.
See also: New findings from Divanovic lab re NAFLD
| Original title: | A BAFF/APRIL axis regulates obesogenic diet-driven weight gain |
| Published in: | Nature Communications |
| Publish date: | May 18, 2021 |