Surgery for a Child with Trisomy 18
Post Date: March 20, 2022 | Publish Date:
A Delicate Balance of Science and Heart
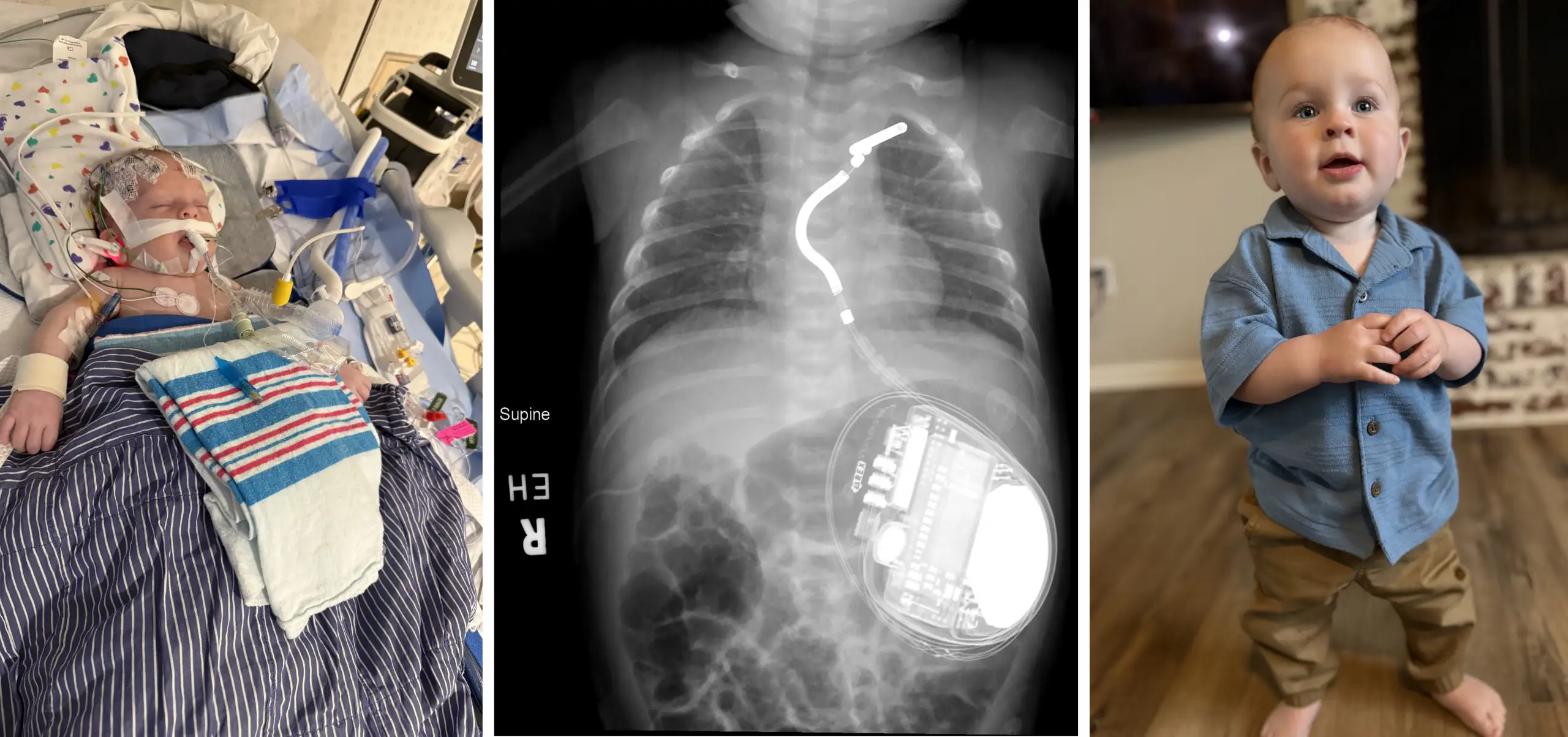
No one can predict how long tiny Thessa Flores will live in the months and years ahead, but thanks to complex surgeries performed at Cincinnati Children’s she is going home to her parents and siblings in California with a heart repaired and cancer cured.
Thessa was born April 14, 2021, with trisomy 18, a rare genetic disorder resulting from having three copies of chromosome 18 instead of two. The disorder causes severe health problems, which can include an underdeveloped ability to breathe, heart defects, liver cancer risks, inability to eat solid food, and other developmental delays.
Trisomy 18, also known as Edwards’ syndrome, happens in about one in 3,300 pregnancies in the United States. About half the babies carried to term are stillborn. Historically, as many as 90% of those who do reach birth do not survive their first year. But improving technologies have helped some children with trisomy 18 live longer.
So, when Tinamarie Costales and John Flores found out about six months into the pregnancy that Thessa had trisomy 18, they faced the first of several difficult decisions.
“The hospital where we planned to have the baby advised us to terminate the pregnancy, and do it soon before it would be illegal,” Tinamarie says. “If we wanted to go through with the pregnancy, all they were willing to do was deliver the baby and send us home with her until she passed.”
After another hospital in California also declined to take on their case, the couple began a wider search, which ultimately led them to Cincinnati Children’s, where surgeons at the Heart Institute have performed cardiac repairs for several children with trisomy 18 and trisomy 13.
In fact, David Cooper, MD, MPH, Medical Director of the Heart Institute, was lead author of a large review of cardiac surgery procedures for these children, published in 2019 in the Journal of the American Heart Association. Five of the co-authors on the paper also were from Cincinnati Children’s, including David Morales, MD, who performed the repair of Thessa’s heart.
Supporting Informed Consent
Knowing that people from around the world seek care from Cincinnati Children’s while carrying a wide range of religious, cultural and personal beliefs, clinicians here work hard not to project their own attitudes onto the life and death decisions parents sometimes must face.


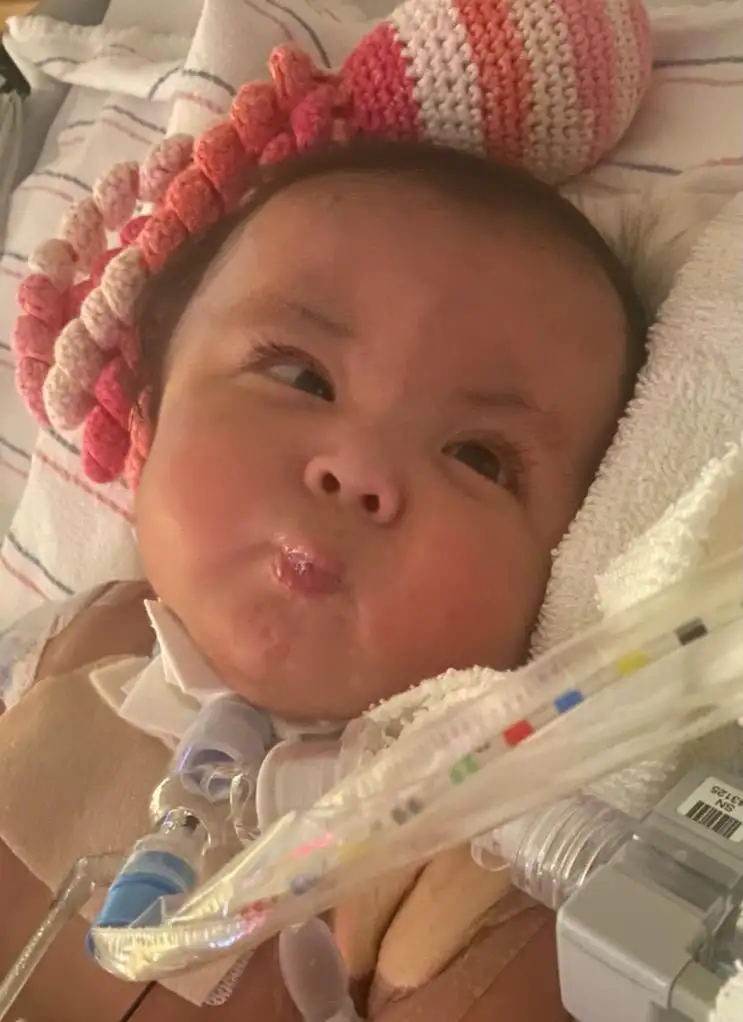

In Thessa’s case, repairing her ventricular septal defect (VSD), a relatively simple cardiac defect, was something the team at Cincinnati Children’s knew they could accomplish. The difficulty revolved around doing a procedure for a child facing so many other health problems.
“We’re not going to use the number of chromosomes you have to determine whether or not you’re going to get surgery. We’re also not going to do surgery just because it’s possible,” Cooper says. “If surgery can provide a meaningful improvement in quality of life, and the family fully understands the burdens they are choosing for their child and themselves, we will honor their decision.”
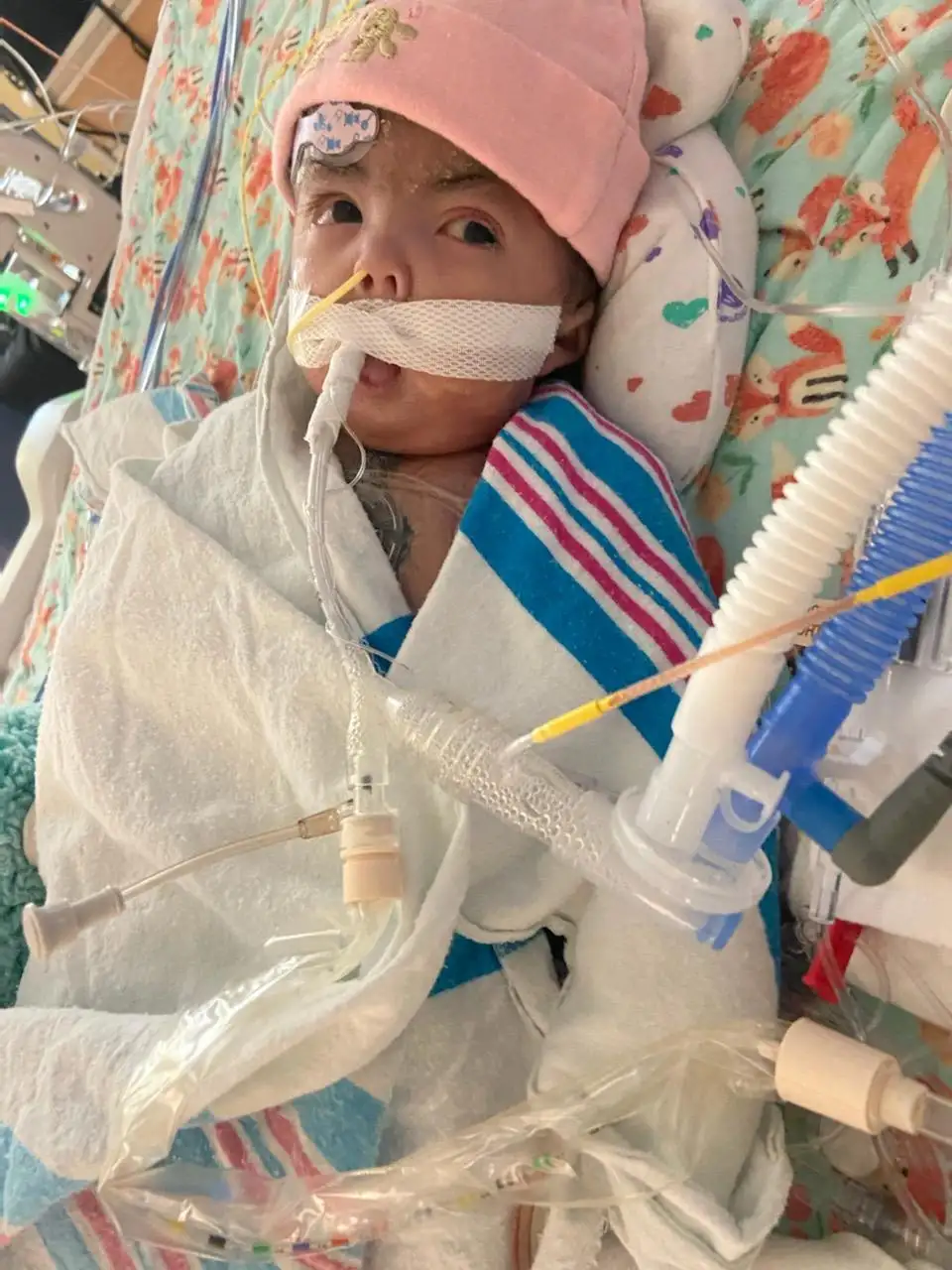
Before doing the operation, the family met with physicians and other care team members who discussed, in detail, the challenges that Thessa would face even if the surgery was a success. Thessa will need a breathing tube and a feeding tube for the rest of her life, and the parents had to be trained how to operate the equipment at home.
The family came to Cincinnati with their eyes fully open, says Tinamarie, herself a nurse practitioner.
“This is Thessa’s life. We just want to be here for her,” she says.
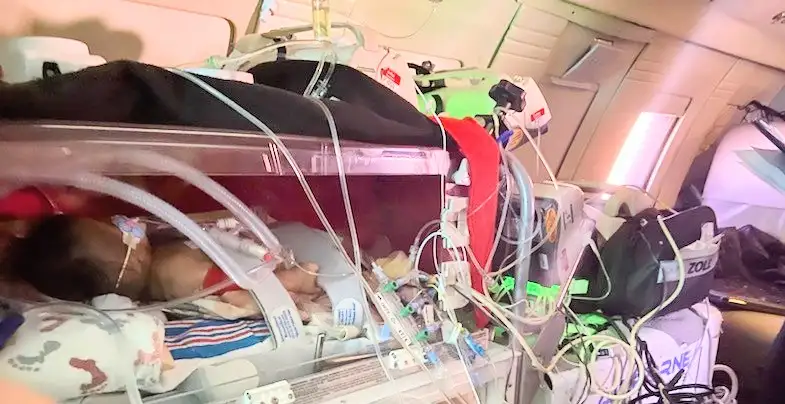
A Logistics Odyssey
Getting Thessa to Cincinnati and back to California required flights aboard medical jet services. Thessa arrived at Cincinnati Children’s in late August, had the surgery in early September and stayed until late February, when she was flown to Miller Children’s & Women’s Hospital Long Beach.
The family had medical insurance to cover many of the bills but making all the necessary arrangements for Thessa’s ongoing care needs was extremely complex. The family did receive considerable charitable support both for the medical flights and for multiple visits back and forth to Cincinnati. Even so, the financial and emotional burden they have accepted has been high.
In addition to her initial heart difficulties, doctors found out during her post-operative recovery that Thessa developed hepatoblastoma, a cancer of the liver, that was also treated at Cincinnati Children’s by oncologist James Geller, MD, and pediatric surgeon Alex Bondoc, MD. She also has hearing loss that required support from audiology experts at Cincinnati Children’s.
But being able to see their child’s face, seeing her smile and feel better has been worth it, Tinamarie says.
The family expressed their gratitude in a letter recently sent to the care team:
“I want to express how grateful we are to all the care that Thessa received while she was there. Thessa came a long way. She had been denied life-saving interventions in California because of her trisomy 18 diagnosis.
Cincinnati gave our family hope of being able to get reunited by offering a full heart repair and all other interventions that Thessa needs so she can be well to come home and meet her family. Having that hearing device will absolutely play a big part in Thessa’s growth and development.
Although it was a sacrifice being so far away from her most of the time, we had a peace of mind that she was getting top-notch care. Our hearts—not just Thessa’s—belong to Cincinnati now.”
Thank You So Much,
Tinamarie and John Flores”
What’s Next?
Cooper says expecting families will still have to make their own decisions about what they should do upon learning that a developing child has trisomy 18. Each case, each family situation is unique.
While all women should try to be healthy during pregnancy, be it receiving all their prenatal care, avoiding harmful substances, eating well, and so on, there’s no specific cause for trisomy 18.
“It’s like getting struck by lightning,” Cooper says. “There is absolutely nothing the mother did wrong or could have done better to prevent the diagnosis.”
While improved technologies are addressing more of the symptoms of children with trisomy 18, a cure appears a long way off. Fetal genetic therapy to “fix” a chromosomal anomaly that affects virtually every cell in the body is not likely anytime soon. But Cooper remains hopeful longer-term for this and other genetic disorders.
“Look how far medicine has come in the past 100 years,” he says. ‘’Who’s to say what discoveries will come decades from now?”
Watch a story aired March 18, 2022, by FOX19
Read a study about liver tumor surgery for children with trisomy 18