Partnering With Families to Improve Emotional Health Care for Children with Chronic Conditions
Research By: Carole Lannon, MD, MPH
Post Date: March 2, 2026 | Publish Date: Dec. 1, 2025
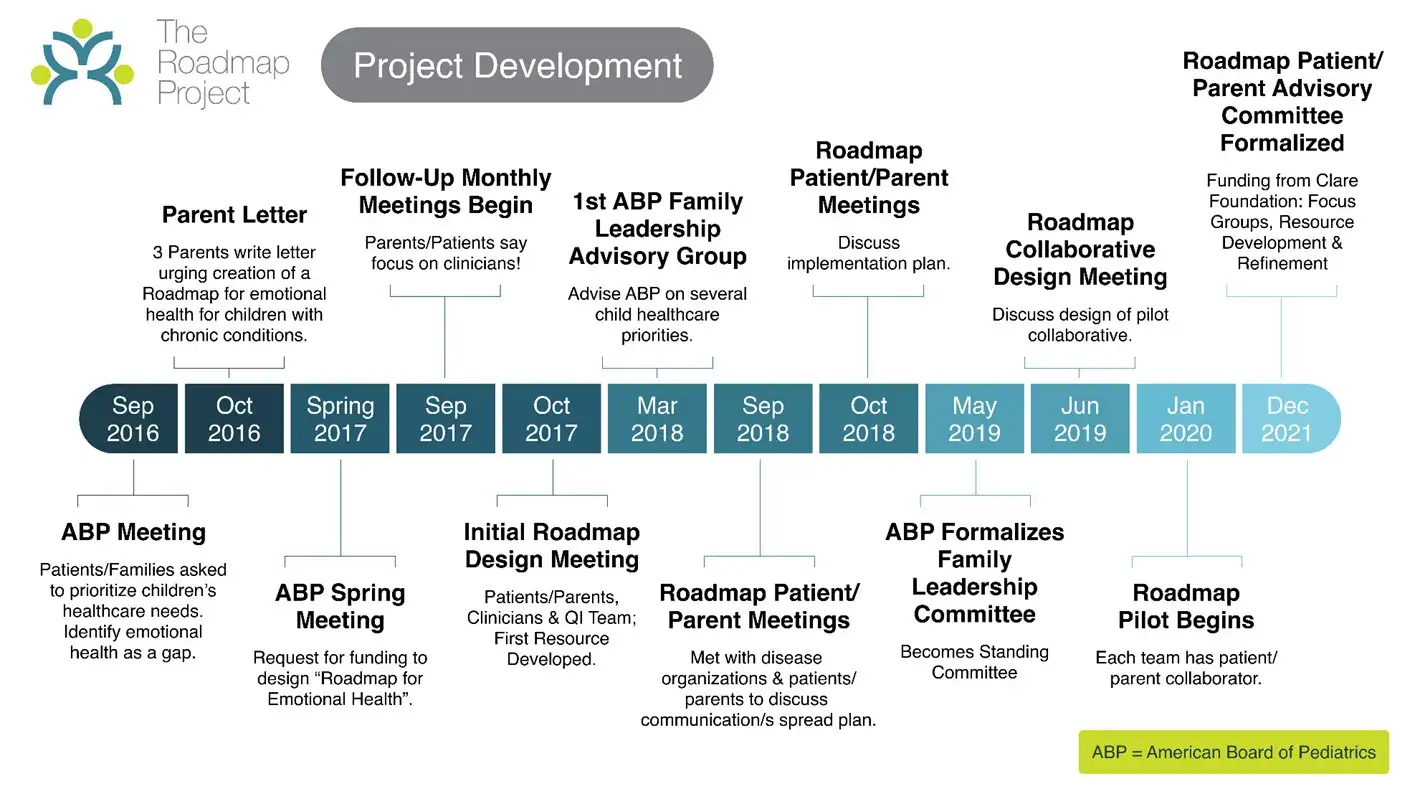
What happens when patients and families help design the very systems meant to support them?
For the Roadmap for Emotional Health Project, the answer is clear: you get an approach that reflects what really matters to patients and families, tools and resources that are easy to use and sustainable, and practical strategies for helping clinicians assess emotional well‑being.
“Partnering With Patients and Families on the Roadmap for Emotional Health,” a recent article published in the Journal of Participatory Research Methods, highlights how collaboration with patients, families, clinicians, and improvement teams can transform care. Engaging families throughout all phases of the project strengthened feasibility, improved the relevance of outcome measures, increased cultural responsiveness, and centered the importance of emotional health support as a standard component for achieving high quality care.
Emotional health is essential to caring for children and adolescents with chronic medical conditions, yet traditional approaches to assessing it have not always included the voices of those affected. Roadmap is changing that. Deep partnership with families has reshaped this improvement project, leading to meaningful gains—such as greater integration of emotional health conversations in clinical visits.
“Projects are more meaningful and effective when they incorporate the diverse voices of individuals who have personal perspectives and direct experience related to the projects intended recipients,” says Robyn Kinebrew, a parent of twins with sickle cell disease and member of the Roadmap Patient and Parent Advisory Group (PPAG), who played a key role in the project’s dissemination and action phases.
Improvement in Action
- Engagement at Every Step Improves Design and Feasibility
Using the Participation Choice Points Model, the team intentionally involved patients and families from early concept development through implementation. Their input helped shape realistic workflows and ensured that Roadmap tools aligned with day-to-day challenges faced by families managing chronic conditions. This early and continuous engagement strengthened project design and feasibility.
- Family-Led Priorities Strengthen Relevance and Equity
By centering patient and family perspectives, the team selected outcome measures that directly reflected what matters most to those receiving care. This approach helped identify gaps and reduce blind spots that can arise when improvement work is designed solely by clinical professionals.
- Co‑Creation Drives Actionable, Real-World Tools
Families played a pivotal role in shaping Roadmap’s practical tools and resources, such as communication guides and emotional health assessment supports that clinicians can use during routine visits. Their input transformed data into actionable strategies, increasing transparency, adoption of emotional health assessment, and long‑term sustainability.
Looking Ahead
The authors emphasize that meaningful partnership is not a one-time effort—it is an ongoing commitment. Future priorities include strengthening infrastructure to support sustained engagement, expanding training that helps clinicians have effective emotional health conversations, and continually refining tools based on ongoing patient and family feedback. As the Roadmap initiative evolves, so will opportunities for shared learning across health systems working to make emotional health support a standard part of care.
Interested in Learning More?
To dive deeper into Cincinnati Children’s quality improvement work, explore the full publication and sign up for the Improvement Insider, a quarterly digest from the James M. Anderson Center for Health Systems Excellence featuring quality stories, emerging research, expert insights, and opportunities to collaborate and learn.
About the Study
In addition to Kinebrew, Cincinnati Children’s co-authors (faculty and parent advisers) also included Bridget Murphy, PhD, Lori Crosby, PsyD, Meghan Roswick‑Didier, and Carole Lannon, MD, MPH.
Don’t Miss a Post:
- Subscribe to the Research Horizons Newsletter
- Follow Cincinnati Children’s Research Foundation on Bluesky, X and LinkedIn
| Original title: | Partnering With Patients and Families on the Roadmap for Emotional Health |
| Published in: | Journal of Participatory Research Methods |
| Publish date: | Dec. 1, 2025 |
Research By

Identifiable gaps in health outcomes piqued my research interests. I now work with patients, families, clinicians and researchers to improve care and outcomes for children and families using learning health networks. These networks, used for improvement and research, can accelerate population health outcomes at scale.