Uganda Study: Penicillin Significantly Reduces Rheumatic Heart Disease Progression in Children
Research By: Andrea Beaton, MD
Post Date: November 16, 2021 | Publish Date: Nov. 13, 2021

Findings, led by experts at Cincinnati Children’s, are an important step in eradicating a disease that affects more than 40.5 million people globally and causes 306,000 deaths annually
A widely available, affordable antibiotic treatment with penicillin significantly reduced the risk of underlying rheumatic heart disease progression in children and adolescents, according to the findings of a clinical study published Nov. 13, 2021, in the New England Journal of Medicine.
The study was led by Andrea Beaton, MD, a pediatric cardiologist at Cincinnati Children’s in collaboration with scientists from Children’s National Hospital in Washington D.C., Murdoch Children’s Research Institute in Australia, and the Uganda Heart Institute. It was dubbed “Gwoko Adunu pa Lutino (GOAL), meaning “protect the heart of a child.”
“This is the first contemporary randomized controlled trial in rheumatic heart disease. The results are incredibly important on their own, but also demonstrate that high-quality clinical trials are feasible to address this neglected cardiovascular disease,” Beaton says. “The GOAL trial is a stunning example of global collaboration, including investigators from six continents, working together to find innovative solutions to reduce the global burden of rheumatic heart disease.”
Rheumatic heart disease is a chronic valvular heart disease caused by rheumatic fever, which develops after an untreated case of strep throat. More than 40.5 million people globally are estimated to be living with rheumatic heart disease, and approximately 306,000 deaths are attributed to it annually.
In low-resource settings, 85% of children with rheumatic heart disease are diagnosed only after the disease has become well-advanced, making medications ineffective and surgical intervention—if available—less likely to succeed. However, the results of the GOAL trial demonstrate that affordable approaches exist that can help more children with rheumatic heart disease.
“We know from previous studies that though it is not always well-documented, sub-Saharan Africa continues to have some of the highest numbers of people with rheumatic heart disease, and the highest numbers of people dying from it,” said Craig Sable, MD, associate chief of Cardiology at Children’s National Hospital and co-senior author of the study. “This study is the first large-scale clinical trial to show that early detection coupled with prophylactic treatment with penicillin is feasible and can prevent rheumatic heart disease from progressing and causing further damage to a child’s heart.”
Penicillin shows promising results
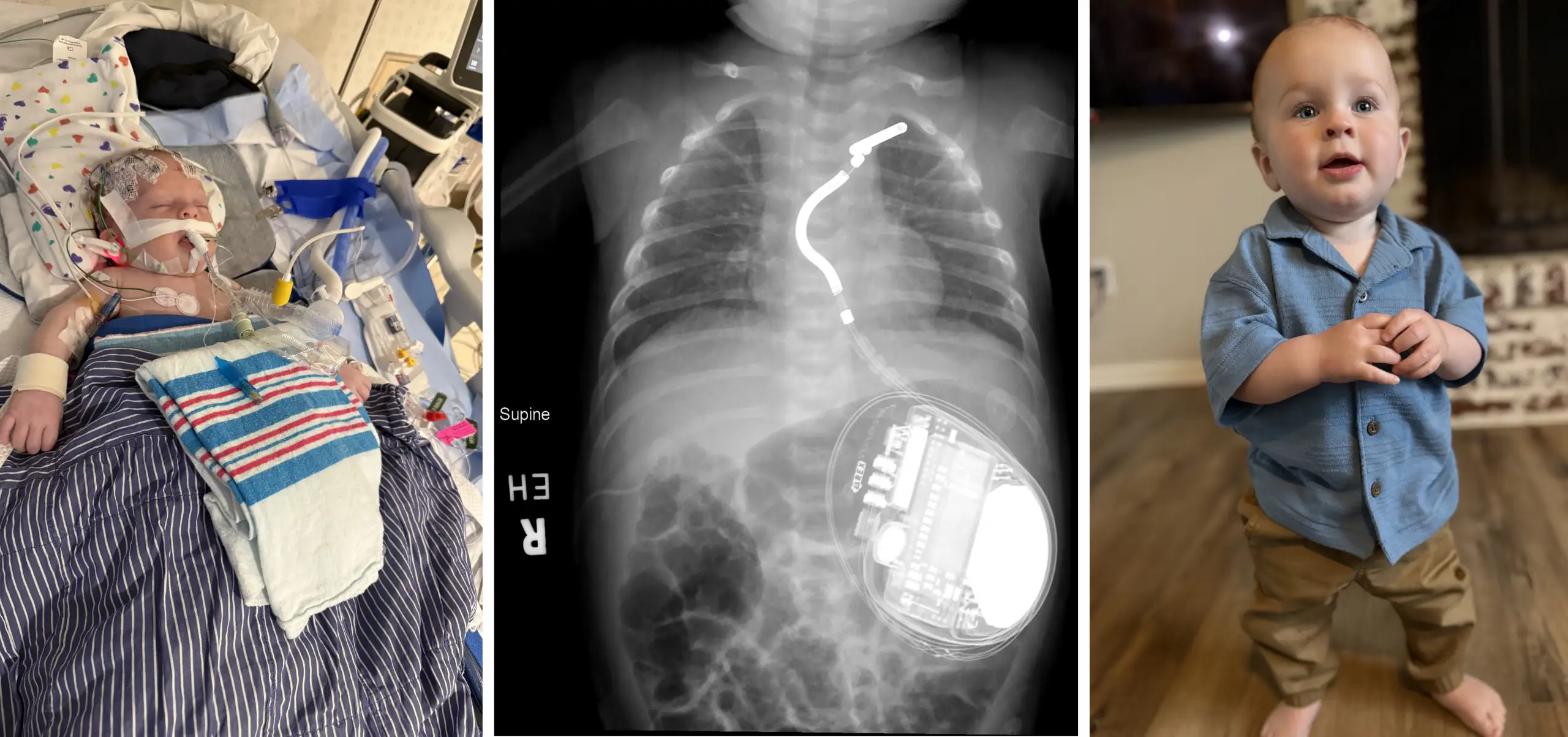
The GOAL trial was conducted in Northern Uganda from July 2018 through October 2020 and involved 818 children ages 5-17 years with latent rheumatic heart disease. The participants either received penicillin injections every four weeks for two years, or no treatment. All participants underwent echocardiography screening, where ultrasound waves produced images of the heart, at the start and end of the trial.
Beaton and co-authors reported that just three participants (0.8%) who received penicillin experienced latent rheumatic heart disease progression after two years, compared to 33 (8.3%) who didn’t receive the treatment. Prior to this study, it was unknown if antibiotics were effective at preventing the progression of latent rheumatic heart disease.
“Our study found that a cheap and easily available penicillin can prevent progression of latent rheumatic heart disease into more severe, irreversible valve damage that is commonly seen in our hospitals with little or no access to valve surgery,” said Emmy Okello, MD, chief of cardiology at the Uganda Heart Institute and co-principal investigator of the GOAL trial.
Next steps: Building up a screening system
These results may not immediately translate into clinical practice in Uganda and other low-resource nations because an enormous amount of infrastructure development remains needed to use echocardiogram screenings as a public health tool, Beaton says. Other barrier to overcome include a lack of retention in care, a lack of available medication, poor access to transportation, social stigma, pain associated with injections, and a limited public understanding of the disease.
Professor Andrew Steer, who leads the Group A Streptococcal Research Group at Murdoch Children’s Research Institute in Melbourne and who served as senior author of the study, said screening for latent rheumatic heart disease was critical to stop progression because heart valve damage was largely untreatable. “Most patients are diagnosed when the disease is advanced, and complications have already developed. If patients can be identified early, there is an opportunity for intervention and improved health outcomes.”
Though there is still work to do, these findings represent an important step in eradicating a disease that disproportionately affects children in low-resource settings around the world, plans for continued research are already in place.
“We have a funded follow-up study called ‘GOAL Post’ from the Trasher Research Fund that will follow these kids for another five years,” Beaton says. “That study will look at the durability of prophylaxis in preventing adverse outcomes as well as determining whether it is safe for children to stop antibiotic prophylaxis once their heart returns to normal. We’re also submitting a study to the National Heart, Lung, and Blood Institute looking at oral versus intramuscular penicillin, which may be a lot more practical in low-resource settings.”
Also contributing to the study were researchers from the University of Cincinnati School of Medicine, Makerere University; Uganda, Children’s National Hospital; Washington, The Royal Children’s Hospital, Telethon Kids Institute, Virginia Tech Carilion School of Medicine, Université de Paris, Instituto Nacional de Saude; Mozambique, Universidade Federal de Minas Gerais; Brazil, Emory University School of Medicine; Atlanta, Starship Children’s Hospital; Auckland, Geisel School of Medicine; New Hampshire, Red Cross Children’s Hospital; South Africa and All India Institute of Medical Sciences.
Listen to Cincinnati Edition show discussing the study
| Original title: | Secondary Antibiotic Prophylaxis for Latent Rheumatic Heart Disease |
| Published in: | The New England Journal of Medicine |
| Publish date: | Nov. 13, 2021 |