A ‘Must Read’—An Update on Asthma Prediction
Research By: Jocelyn Biagini, PhD | Lisa Martin, PhD | Gurjit Khurana Hershey, MD, PhD
Post Date: January 21, 2026 | Publish Date: Dec. 15, 2025
Identifying ways to help vulnerable children who are at risk of developing asthma can only be accomplished when we understand what factors promote asthma. A recent study in Pediatric Allergy and Immunology published December 15, 2025, shows that neighborhood factors—which can be influenced by societal changes or physical relocation—are just as accurate in predicting asthma risk as self-reported race.
“This finding is important because it tells us that the environment around where a child lives can impact their risk of becoming asthmatic. Understanding this can help us design interventions to improve the environment in at risk neighborhoods,” says Gurjit Khurana Hershey, MD, PhD, corresponding and senior author of the study.
In fact, this study was impressive enough that it was recently selected by the European Academy of Allergy and Clinical Immunology’s Junior Members Assembly as a “JM Must Read” paper for allergy trainees. An editorial comment will be published in an upcoming journal issue.
How do we predict asthma?
Identifying children who are at risk of developing asthma is important to help identify ways to prevent the disease.
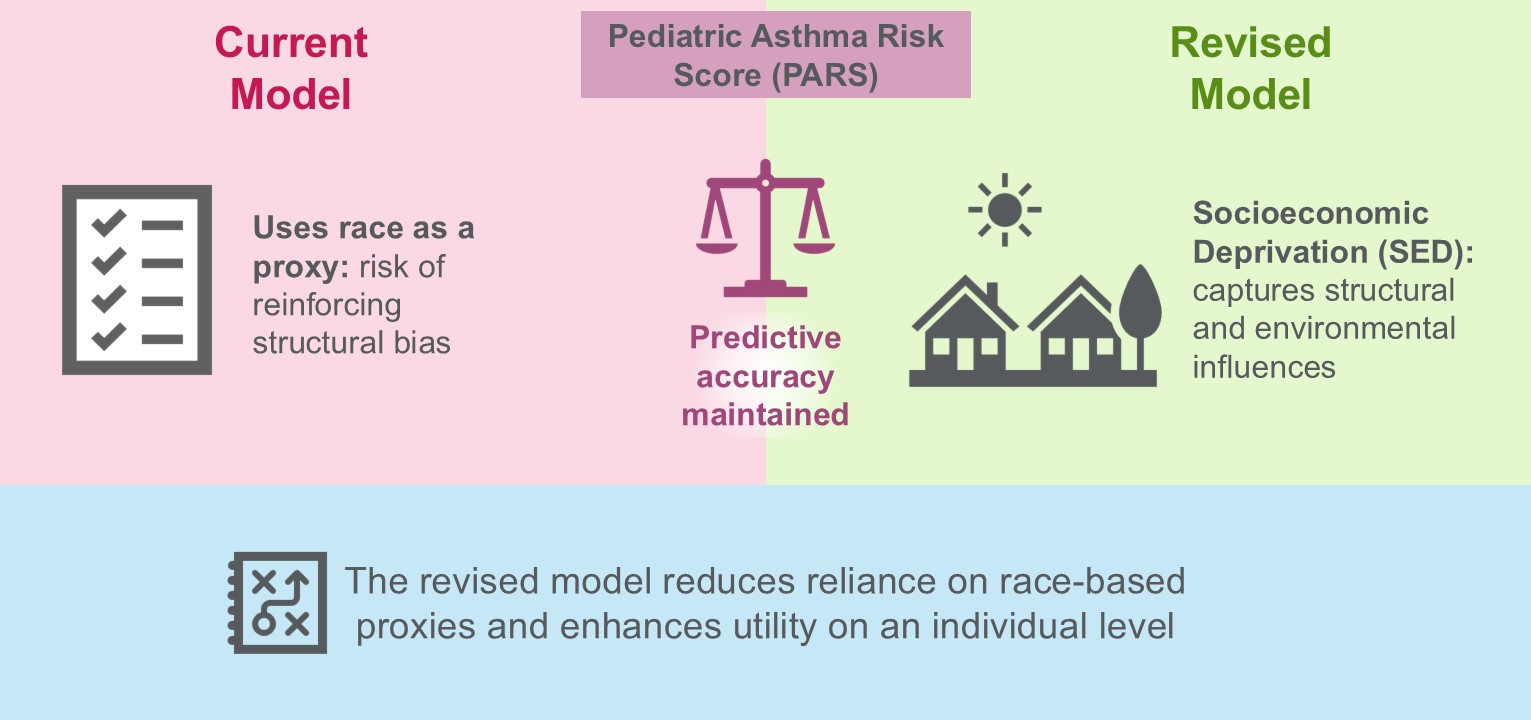
In 2018, researchers at Cincinnati Children’s developed a quantitative risk score to estimate asthma development which can be easily and quickly used in a clinical office setting. This Pediatric Asthma Risk Score (PARS) is determined using six factors, including parent-reported Black/African American race.
While PARS was originally developed from two cohorts, including one in Cincinnati, in 2023 researchers validated its generalizability with 10 separate cohorts across the United States that were designed to study asthma. Over the years, PARS has gained global adoption from clinicians, parents, students and researchers in at least 166 countries.
However, racial disparities in asthma have been documented for decades and there has been a call to remove race from medical practice. Indeed, race was originally used in PARS as a proxy for multiple unidentified factors, but “race” itself lacks biological meaning. Rather, “race”—especially as it has been used in PARS—likely reflects multiple factors, including cultural, socioeconomic, heritable, environmental, and social factors.
Updating asthma prediction using lived environment
Experts have not yet reached agreement on the most appropriate alternative to race for determining asthma risk. Composite indices—such as socioeconomic deprivation (SED)—combine multiple dimensions of a person’s socioeconomic position, including neighborhood and environment, into a single variable. Therefore, using a SED index in place of race may help better explain why asthma risk differs between groups.
In the study led by Jocelyn Biagini, PhD, 11 SED indices were tested for replacement of race in PARS using two cohorts, the Cincinnati Childhood Allergy and Air Pollution Study (CCAAPS) and the Mechanisms of Progression of Atopic Dermatitis to Asthma (MPAACH) cohorts. All 11 SED indices performed similarly to race in the model and likely captures much of the signal race previously represented.
Importantly, most children (93%) did not change asthma risk category when SED was used in place of race in PARS. The small subset of participants who did have a change in their asthma risk category showed no clear pattern in the change in risk, nor did they have any obvious demographic or environmental exposure driving the change in their PARS score.
Moving Forward
Co-authors of this study encourage the replacement of race with SED in PARS. This may better classify the socioeconomic position and environmental exposures of a child, which will enhance the utility of the tool on an individual level. In the future, co-authors highlight the opportunity to test the replacement of race with SED in a more geographically diverse study.
It is important to note that SED indices, which use census data, outperform the Global Gridded Relative Deprivation Index (GRDI), which is much less precise in assessing deprivation at a particular address. In fact, GRDI and SED were not correlated in any of the testing and race still performed better than GRDI in PARS. Therefore, it will be critical to find better global solutions.
About the study
Jocelyn Biagini, PhD was the first author of the study. Co-authors included experts from the divisions of Asthma Research and Human Genetics. Funding sources included two grants from the National Institutes of Health (R01ES011170 and U19AI070235).
Don’t Miss a Post:
- Subscribe to the Research Horizons Newsletter
- Follow Cincinnati Children’s Research Foundation on Bluesky, X and LinkedIn
| Original title: | Socioeconomic deprivation performs equally to race in the Pediatric Asthma Risk Score |
| Published in: | Pediatric Allergy and Immunology |
| Publish date: | Dec. 15, 2025 |
Research By

Our research focuses on understanding the epidemiology of asthma, with an emphasis on how environmental exposures and genetic factors interact to drive asthma risk.

I’m a researcher interested in statistical genetics, complex traits, statistical rigor and allergic disorders. I work with various collaborators to evaluate how genetics may contribute to patient outcomes.

My lab combines epidemiologic, basic, translational and clinical research approaches to answer fundamental questions related to childhood asthma, atopic dermatitis, food allergy and allergic rhinitis.







