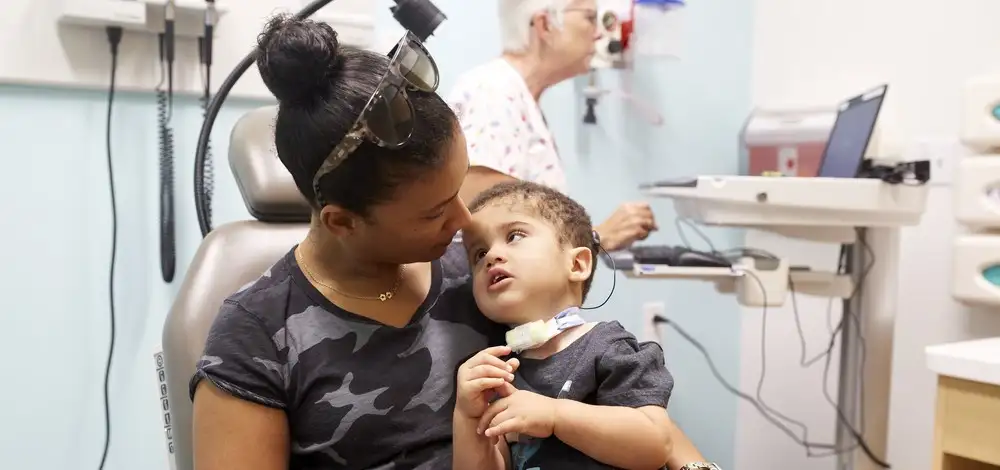A Logic Model Approach to Integrating Trauma-Informed Care
Research By: Sarah Zawaly
Post Date: July 22, 2025 | Publish Date: Sept. 26, 2024
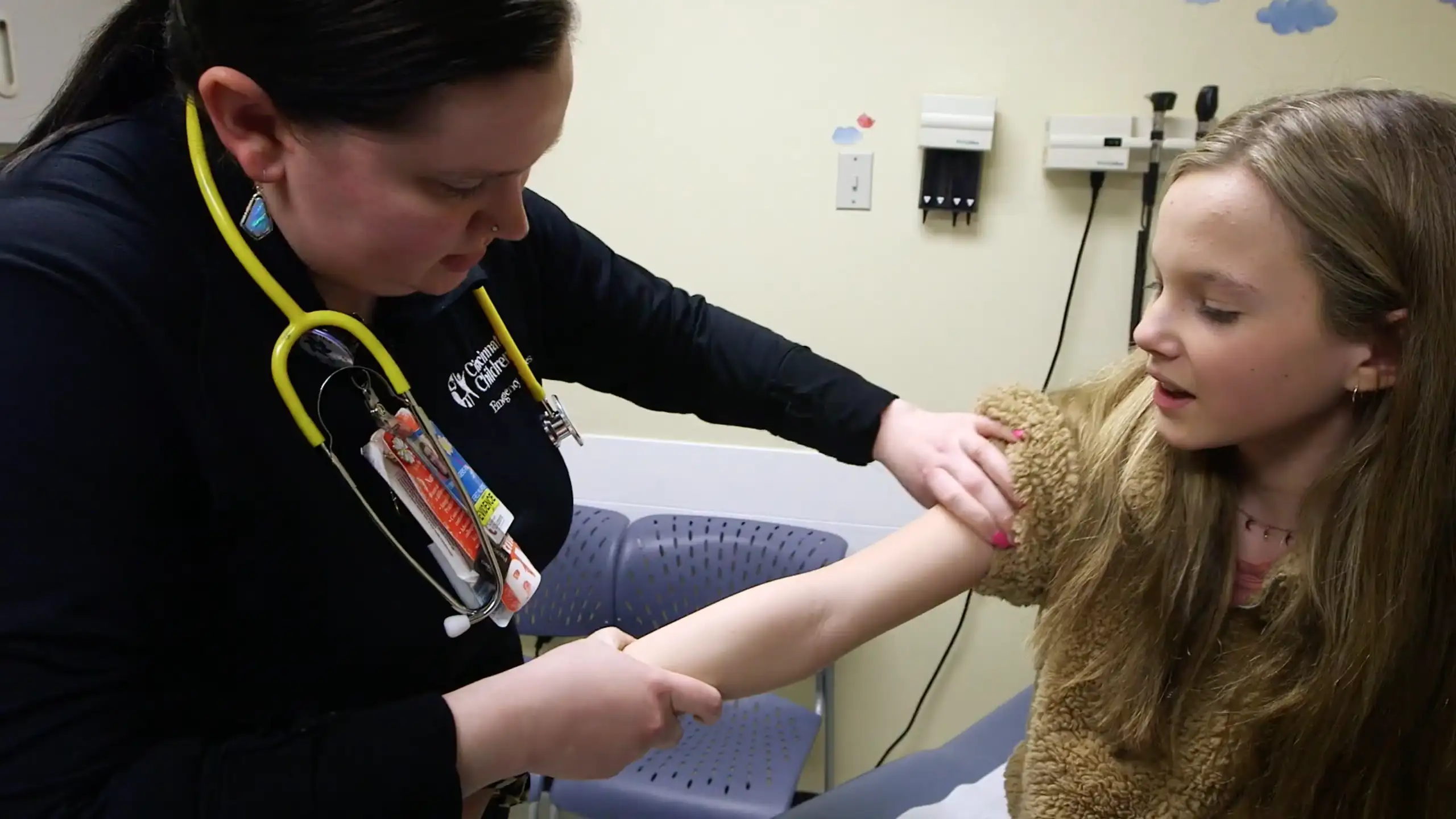
Providing trauma-informed care requires a layered approach that spans every level of a health system—from individual patient interactions to organizational culture and community partnerships.
At Cincinnati Children’s, an interdisciplinary team of researchers—working in partnership with the collective impact group, Joining Forces for Children—developed a trauma-informed care (TIC) logic model. This framework guides the steps necessary to become a trauma-informed organization.
“We understand that trauma is common,” says Sarah Zawaly, MSW, a clinical program manager in the Cincinnati Children’s Mayerson Center for Safe and Healthy Children. “It impacts patients, families and staff—all of us. Trauma dysregulation and its signs and symptoms or a lack of understanding and miscommunication impacts the whole system.”
The logic model outlines steps to organize trauma-informed care that promotes child health and well-being by fostering an optimal healing environment—one that:
- Promotes protective factors
- Reduces the impact of adverse childhood experiences (ACEs)
- Improves health equity
- Centers the voices of patients and families
Cincinnati Children’s uses the model to train hospital departments, employers, schools and other healthcare organizations across the Cincinnati region and beyond.
What is a Trauma-Informed Healthcare System?
The TIC logic model—published in Hospital Pediatrics by Zawaly and colleagues Pratima Shanbhag, MD, MPH; Anita Shah, DO, MS; and Elizabeth Lanphier, PhD, MS—defines the foundational components of a trauma-informed healthcare system. These include:
- Realizing the widespread impact of trauma and understanding potential paths for recovery
- Recognizing the signs and symptoms of trauma (in pediatrics, this includes children, families and healthcare staff)
- Responding by integrating knowledge about trauma into policies, procedures and practices
- Seeking to actively resist re-traumatization
The strategic framework includes short- and long-term goals mapped over a five-year period.
“While education is one important step, we carefully consider next steps—using quality improvement and leadership engagement to truly embrace the definition of becoming a trauma-informed organization,” says Shah, an attending physician in the Division of Hospital Medicine.
A Community-Wide Effort
The logic model outlines strategies in three core areas: workforce development, prevention and intervention, and hospital policies and procedures. Inputs include:
- Community partnerships and resilience-building efforts
- Departmental workgroups
- Leadership support
- Patient and family feedback
- Ongoing research
The Cincinnati Children’s TIC task force meets monthly and includes members from across the health system.
“This is a part of delivering excellent care,” Zawaly says. “It overlaps with many other initiatives and priorities.”
The task force uses a broad definition of trauma—including both medical and community-based trauma—which opens the door for TIC practices in many settings. Shanbhag, a child abuse pediatrician at the Mayerson Center for Safe & Healthy Children and a Trauma-Informed Champion with the American Academy of Pediatrics, partners with Zawaly to extend trauma-informed training to schools, libraries, recreation centers, and more.
Cincinnati Children’s offers:
- A free online learning series for community members
- On-demand TIC digital learning modules for health system staff
- A three-part training program for hospital departments and community partners on request.
“There are many people across our organization committed to spreading TIC to a variety of settings,” Zawaly says. “Dedicated individuals at the grassroots level and committed leadership reflect the collective ownership. That’s what makes it sustainable, so many people are passionate about and focused on trauma-informed care.”
Healing Through Human Connection
A strengths-based approach complements TIC training and encourages providers to recognize and build on the positive traits of the children and families they serve.
“If we can help a caregiver nurture a child’s strength at home,” Shanbhag says, “that can become a protective factor that supports the child’s long-term resilience.”
Clinicians also learn how every interaction with a patient or family can be an opportunity for healing, Zawaly says. Trauma-informed care includes self-awareness, too. Providers are encouraged to recognize their own emotional responses and know when they need support.
“Clinicians experience trauma, too,” Zawaly says. “If they don’t take time to recharge and care for themselves, it can lead to burnout.”
The TIC model also helps providers navigate difficult communication moments with families.
“It helps me pause, reflect on my own biases and listen more closely when a family feels unheard,” Shah says. “That’s when real partnership begins.”
What’s Next?
The logic model authors encourage organizations to embed trauma-informed practices into existing programs—such as annual safety training—to increase knowledge and move toward sustainable change. Organizations can use existing tools—like employee engagement surveys—to monitor their TIC progress, identify needs related to psychological safety and power dynamics, and inform continuous improvement.
To learn more, access online training or schedule a trauma-informed care session for your team:
- Call the Mayerson Center at 513-636-7233
- Contact Sarah Zawaly at zawaly@cchmc.org
- Read about our training for professionals
Don’t Miss a Post:
- Subscribe to the Research Horizons Newsletter
- Follow Cincinnati Children’s Research Foundation on Bluesky, X and LinkedIn
| Original title: | A Logic Model Approach to Trauma-Informed Care |
| Published in: | Hospital Pediatrics |
| Publish date: | Sept. 26, 2024 |
Research By