What Will It Take to Make EHR a Partner Instead of a Burden?
Post Date: March 25, 2022 | Publish Date:

Clinicians who have burned uncounted hours documenting their work into their patients’ electronic health record (EHR) may not like Kevin Johnson, MD, MS, very much. As both a pediatrician and an expert in computer sciences, he helped develop some of the early clinical information systems that have since evolved into behemoths like EPIC.
Johnson, now vice president for applied informatics for the University of Pennsylvania Health System, is well aware of the many entanglements that make today’s EHR experience a serious source of burnout for clinicians. His message: It wasn’t supposed to be this way, and it doesn’t have to stay this way.
In fact, he predicts a new wave of transformation in digital health technologies that could make rapid progress on four critical goals: Improving outcomes, reducing costs, enhancing the patient and family experience, AND improving the clinician’s day-to-day experience with documentation.
Johnson discussed the evolution of the EHR and its future directions on March 22, 2022, as part of Cincinnati Children’s speaker series Envisioning Our Future For Children. The series has hosted presentations from widely-known experts in pediatric health fields including Donald Berwick, MD, founding CEO of the Institute for Healthcare Improvement, Jim Yong Kim, MD, co-founder of Partners in Health, and Victor Dzau, MD, president of the National Academy of Medicine.

Long journey, not there yet
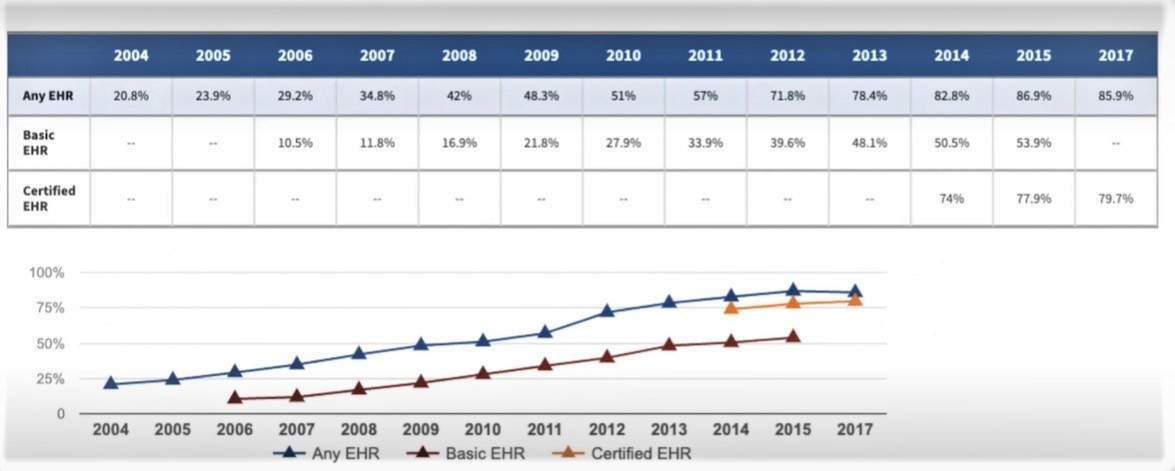
While the potential benefit of moving medical records from paper to digital systems was hailed as the wave of the future since the 1990s, by 2008, only about 4% of clinicians were using fully functional EHR systems, Johnson says. The pace picked up after the adoption of the HITECH Act of 2009, but even with digital records now part of about 90 percent of physicians’ routine, the change has only just begun living up to some of the early promises.
Studies published as recently as 2020 lamented that pediatricians were spending two minutes documenting their work for every minute actually spent with patients. Stagnant innovation in terms of user-friendliness resulted in surveys giving EHR systems an “F” for usability while Google’s search function earned an “A” and bank ATMs earned a “B” on the same rating scale.
Change on the horizon
Improvements are coming, including a “25×5” movement launched in 2021 by a number of top health organizations to cut documentation to just 25% of a clinician’s time by 2025.
“We are now on the same page with many of the disciplines that could make the EHR a true partner in care,” Johnson says.
In the years to come, the EHR will be a more effective tool for supporting precision medicine and many other quality improvements. It could help advance understanding of biosocial pathogenesis, a field that’s exploring the blend of biological health risks and social determinants of health.
Instead of patient records documenting just one person’s care journey, the data from better integrated systems can shed light of population health issues and be used to target health improvement spending beyond the confines of hospitals and medical offices.
In addition, advances in EHR technology have the potential to support better equity in healthcare access and outcomes. Part of the change facing traditional pediatric practices will be that other stakeholders will become more directly connected to the EHR—including school nurses, community pharmacists, even the patients and the wearable devices they use to track health measures.

Johnson urged pediatricians to learn more about three emerging trends:
- Edge computing and the changes in data sharing that are coming with 5G will become topics that doctors will need to understand.
- The blockchain concepts behind cryptocurrency will influence, and possibly transform, how medical information is protected, how bills are paid, and more.
- Expanding “agency.” Be it smart devices, better-connected school nurses, or the establishment of telemedicine, physicians and hospitals will no longer be the only sources of truth for the contents of a person’s digital health record.
Stay tuned for more speakers. Coming Oct. 4: Diana Bianchi, MD, Director, Eunice Kennedy Shriver National Institute of Child Health and Human Development
Watch Dr. Johnson’s full presentation