Cincinnati Children’s Launches 6 COVID-19 Research Projects
Post Date: May 26, 2020 | Publish Date:
Work to Focus on Developing Vaccine Nanoparticles, Studying Effects on Heart Tissue, Data Analysis, and How Virus Affects Foster Youth, ADHD, and Sickle Cell Disease
From developing a potential vaccine based on nanoparticles to tracking how the pandemic has disrupted life for foster children, scientists at Cincinnati Children’s have launched six projects aimed at understanding and defeating the virus that causes COVID-19.
The projects, announced May 25, 2020, have received a combined $450,000 in internal funding from Cincinnati Children’s.
“These projects were selected by a panel of senior research leaders at Cincinnati Children’s from more than 35 proposals,“ says Hector Wong, MD, interim Chair of the Department of Pediatrics and interim Director of the Cincinnati Children’s Research Foundation. “We deeply appreciate the swift, creative and enthusiastic response of our faculty to this global health crisis and we look forward to seeing the results of these important research efforts.”
The projects are:

Construction of SARS-CoV-2 pseudovirus nanoparticles as a COVID -19 vaccine candidate
Ming Tan, PhD, is a virology expert who has developed “P particles” and “S particles” for use against norovirus, rotavirus, and other infectious diseases, in collaboration with his colleague Xi Jiang, PhD. Now they are engineering nano-sized pieces of the SARS-CoV-2 pseudovirus for potential use as a vaccine ingredient to trigger the body’s natural immune response to produce antibody against COVID-19.
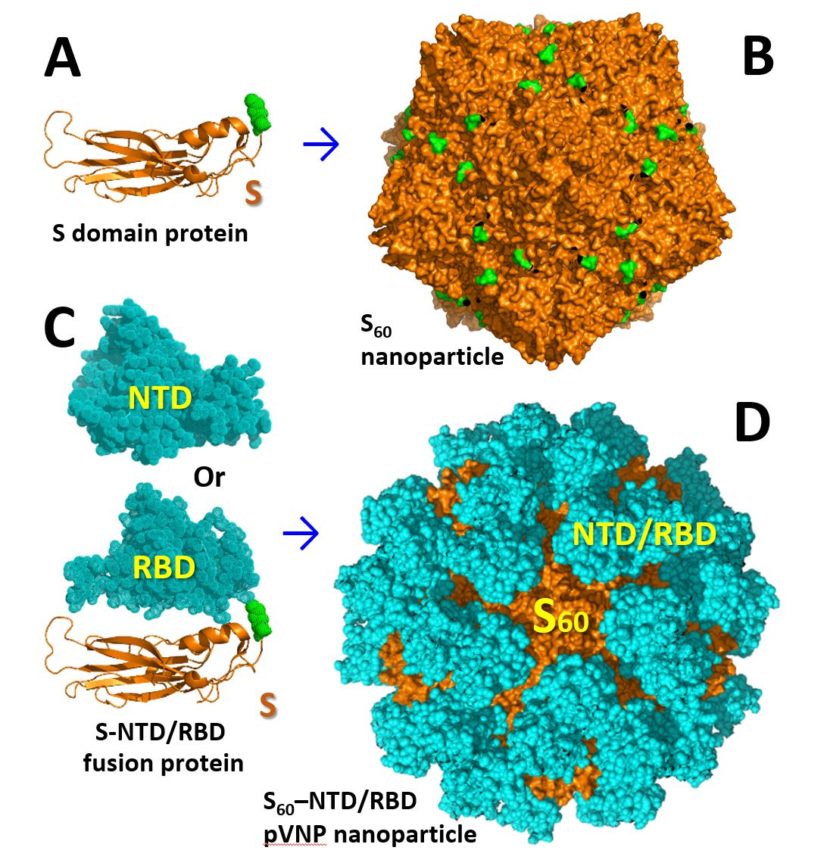
“Lately we have invented a patented nanotechnology to make pseudovirus nanoparticles (pVNPs) for vaccine development,” Tan says. “This is based on our innovative S60 nanoparticle.”
The S60 particle was built as a virus-like platform to display antigens of other viruses for novel vaccine development. This concept has been proven in principle by developing pVNPs against rotavirus and influenza virus.
“Based on these past successes, we propose in this project to generate two new pVNPs displaying the receptor binding domains of SARS-CoV-2 virus, and mix them as a bivalent COVID-19 vaccine candidate,” Tan says.
This project could take a year or more to complete for two important reasons:
Once small quantities are produced, mouse studies and human clinical testing will be needed to confirm that the vaccine works, and to determine the correct dose needed to prevent disease while maximizing safety.
Meanwhile, the stability, or “shelf life,” of the nanoparticles must be determined. To do this, the team plans to store particles at -80℃. -20℃, 4℃, and room temperature for various time periods of up to 12 months.
In previous work, Tan has reported that the S60 nanoparticles lack the ability to replicate, and thus pose less risk than traditional vaccine-making methods. Also, pVNPs can be manufactured via a recombinant protein production system that offers lower costs and higher speed than traditional vaccine production methods.
Tan’s efforts could lead to a vaccine developed here at Cincinnati Children’s—a long-time leader in vaccine research—or could be melded into one or more of the 90-plus vaccine projects launched to protect the world from future waves of COVID-19.
See related research:
Pharmaceutics: Norovirus Capsid Protein-Derived Nanoparticles and Polymers as Versatile Platforms for Antigen Presentation and Vaccine Development
Vaccine: Immune response and protective efficacy of the S particle presented rotavirus VP8* vaccine in mice
PLOS Pathogens: Molecular basis of P[II] major human rotavirus VP8* domain recognition of histo-blood group antigens
Vaccines: Parenterally Administered P24-VP8* Nanoparticle Vaccine Conferred Strong Protection …
Journal of Virology: The P Domain of Norovirus Capsid Protein Forms a Subviral Particle That Binds to Histo-Blood Group Antigen Receptors


Investigation of cellular and signaling determinants of COVID-19-induced human cardiomyopathy
Beyond assaulting the lungs, scientists have discovered that the novel coronavirus also can cause significant heart damage that has proven fatal in some cases and could affect survivors for the rest of their lives.
Now Jeffery Molkentin, PhD, Director of the Division of Molecular Cardiovascular Biology and Co-Director of the Heart Institute at Cincinnati Children’s, is teaming up with Steve Standage, MD, an expert in critical care medicine to lead a multi-center research effort to understand how the virus interacts with heart tissue at the molecular level.
The results could help researchers develop tests and treatments to help prevent deaths and reduce potential future heart complications caused by the new virus. But first, the team needs tissue samples to study.
”We desperately need explanted cardiac tissue from COVID-19 patients to investigate these potential pathophysiologic mechanisms in order to effectively stratify distressed patients and identify new treatments,” Molkentin and Standage say.
Early study of COVID-19 already has revealed that the new virus causes cardiovascular problems similar to cases reported in the SARS (2002) and MERS (2012) outbreaks. The team breaks the complications into three categories:
- Oxygen deprivation associated with direct lung damage but also due to widespread blood clotting, both of which will indirectly damage heart tissue.
- A hypothesized “cytokine storm” that appears to reflect an overzealous immune response in some patients, producing a type of shock that affects the heart.
- Possible direct viral infection of cells in the heart either causing selective cell death or direct vascular defects leading to diffuse coagulation within the heart.
However, considerable analysis of heart tissues, collected from autopsies, is required to determine precisely how these types of damage occur, which in turn will help experts develop more-precise ways to treat those problems. Early genetic studies have already revealed as many as 60 molecular pathways affected by COVID-19 that may have “druggable” targets, meaning that existing medications are known to influence those pathways. But which of these might be best to pursue?
The Molkentin laboratory has been studying such pathways for 22 years while Standage has been studying cardiac septic shock for 10 years. Their goal is to generate a biobank of heart tissue to conduct further analysis.

Global Incidence, Prevalence, and Impact of COVID-19 in Children with Sickle Cell Anemia
The medical community has known for some time that viral infections can trigger acute chest syndrome and other complications of sickle cell disease (SCD), some of which can even lead to death.
In fact, when children with SCD are infected by influenza, they have a 56-fold increased risk of hospitalization and are more likely to require intensive care compared to children without SCD.
Small wonder then that the emergence of COVID-19 sparked concern among experts at Cincinnati Children’s who have devoted years to improving outcomes for this inherited condition here in Cincinnati and across the world.
Sickle cell is the most commonly detected condition by newborn screening in the US, where it affects about 100,000 people. But the disease is much more common in Africa, and much more deadly. In sub-Saharan Africa, nearly 1,000 children are born each day with SCD and 50-90% of those children die before reaching age 5.
Patrick McGann, MD, MS, has been studying this disease for years. He has been a leader in establishing that hydroxyurea treatments can be safely used here and in Africa as a more affordable, easier to tolerate alternative to controlling pain and other sickle cell symptoms with repeated blood transfusions.
Now he plans to work with Charles Quinn, MD, MS, Medical Director of the Pediatric Sickle Cell Program at Cincinnati Children’s, and Russell Ware, MD, PhD, Director, Division of Hematology and the Global Health Center, to learn more about how COVID-19 is affecting the SCD population here in Cincinnati, in Africa, and in the Caribbean.
They plan to use blood samples that are already being collected within existing research studies to test for active COVID-19 infection and for the presence of COVID-19 antibodies to document prior exposure. Their data will help establish how much risk people with sickle cell face from a COVID-19 infection, how severe their illness is if they become infected, and what can be done to reduce that risk.
“The potential burden of COVID-19 has implications beyond those of acute infection,” McGann says. “Due to worldwide quarantines, healthcare resources are becoming limited even in well-resourced settings. This will undoubtedly have an impact upon the sickle cell community in the US and across the world as the availability of blood transfusions and timely access to emergency healthcare both are likely to become limited.”
In the U.S., the sickle cell community already has begun working on emergency plans in case disruptions to the blood supply disrupt needed access to monthly blood transfusions. Such challenges will become even more serious as the pandemic spreads in low-resource nations.

Impact of COVID-19 In Adolescents With and Without ADHD
Families facing job losses. Long weeks stuck at home instead of seeing friends at school. Major disruptions in routines and traditions. Widespread fear and anxiety about the future. Non-stop news.
The disruptions caused by the COVID-19 pandemic have been immense.
“The COVID-19 pandemic presents tremendous challenges to child and adolescent well-being. With the implementation of social distancing, direct human contact has become highly restricted, with most activities that typically occupy youths’ lives – school, extracurriculars, and time with friends – now limited to electronic-based platforms,” says Stephen Becker, PhD, a clinical psychologist at Cincinnati Children’s who has studied attention-deficit/hyperactivity disorder (ADHD) for most of his career.
“However, the experience of the COVID-19 pandemic and its consequences are likely to be particularly magnified and salient in youth with pre-existing mental health and neurodevelopmental risk, such as ADHD,” Becker says.
His team is expanding an existing study involving more than 260 teens with and without ADHD to identify COVID-19 impacts on emotions, sleep, academics, media use, family relations and more. Comparing how youth with and without ADHD cope with the pandemic may reveal predictive signs that can help professionals determine when and how to intervene.
Before the pandemic struck, this group of teens had already been followed across five time points. Now the group will be asked to participate in evaluations at four more time points since the pandemic began.
Becker will be working with colleagues in Virginia and California who were involved in the initial project.
“It is our goal for this project to advance science while also being directly helpful to participants and other families during this challenging time,” he says.


Impact of COVID-19 Telehealth and Service Disruption on Foster Youth
Children growing up in the foster care system have experienced vast amounts of disruption to their lives. They have long needed more extensive mental health, educational and medical support than many communities can provide.
Now, the care and support systems that foster youth depend upon are facing new disruptions from the COVID-19 pandemic, according to Mary Greiner, MD, MS, Medical Director for the CHECK Foster Care Center, and Sarah Beal, PhD, a developmental psychologist at Cincinnati Children’s.
“Our children are not able to access the supports they have traditionally relied on. They are out of school physically and many struggle to participate in remote learning, particularly those with special education requirements,” Greiner and Beal say. “Many have lost early intervention and developmental services from both the health care system and the community. Mental health services have been difficult to establish and continue, particularly more intense in person programming, such as partial hospitalization. They may not be receiving community psychiatry supportive treatment (CPST) or mentorship during this time. Even health care visits have been disrupted.”
All of these disruptions can lead to bad outcomes for these children.
The biggest single type of pandemic response affecting foster youth has been the explosion in use of telemedicine services to allow remote access to professional services. “However, we are realizing that there is a lot we don’t know about delivering virtual care to this population,” Beal says.
From lack of consistent internet access to regulatory barriers to personal levels of comfort with remote communication, a variety of issues related to serving foster youth via telemedicine need much more study.
For the next nine months, the team plans to survey more than 200 families, conduct mock telehealth visits, and gather other data to measure the impacts of COVID-19 on this population and to recommend best practices for the many agencies involved in supporting foster youth.
“Understanding where there are gaps and who needs additional support will help us make informed decisions as services and resources begin to open up again in Ohio,” Greiner says.

COVID-Miner: Leveraging Artificial Intelligence to Facilitate Early Detection of Coronavirus Infection and Deterioration in the Pediatric Population
This pandemic is big and fully understanding its impacts will require plenty of “big data.” That’s where biomedical informatics expert Yizhao Ni, PhD, plans to help.
Ni has extensive experience in using the concepts of natural language processing (NLP) and machine learning to help computers “learn” as a form of artificial intelligence.
Ni already has developed sophisticated computerized algorithms that are helping doctors and scientists explore information buried in electronic health records, particularly from clinical narratives. This work is helping improve intensive care services, spot hard-to-track medication complications, and more.
Now Ni plans to develop a tool called COVID-Miner that has two components. The tool will use NLP technology to extract vital risk factor information about COVID-19 from near-endless streams of medical information flowing into hospitals all around the world. It also will use machine learning concepts to use the gathered information to predict COVID-19 infection and deterioration in patients in ways that can help mitigate viral spread and limit mortality.
The idea for this project emerged soon after the White House and leading research groups launched the COVID-19 Open Research Dataset (CORD-19), which is a resource of over 59,000 scholarly articles about COVID-19 and other coronaviruses.
“By exploring this large collection with our text search engine, we can develop a comprehensive set of risk factors for coronavirus infection in the pediatric population, which ultimately can be disseminated to other centers,” Ni says.
The project is expected to take at least a year. The goal will be to have a system that clinicians can use to track and plan treatments for individual patients as the virus spreads in the months to come.