15-Site Trial to Compare Telehealth Cognitive Behavior Therapy Alone and with Medication to Prevent Migraine in Youth
Research By: Scott Powers, PhD
Post Date: July 26, 2022 | Publish Date:
Researchers at Cincinnati Children’s have been approved for a $12.9 million funding award by the Patient-Centered Outcomes Research Institute (PCORI) to lead a multi-center study to compare two methods for helping adolescents manage their migraine pain.
The project, to be led by Scott Powers, PhD, Division of Behavioral Medicine and Clinical Psychology, will explore how well cognitive behavior therapy (CBT) delivered by telehealth reduces headache days and disability from migraine compared to CBT telehealth plus a prevention medication (amitriptyline). Participants will be youth with migraine from ages 10 to 17.
Cincinnati Children’s has played a large role in demonstrating the value of non-medication approaches to treating migraine. Among the key findings from more than a decade of research:
2013: Powers and the Headache Center team at Cincinnati Children’s published findings in the Journal of the American Medical Association (JAMA) that showed cognitive behavioral therapy with amitriptyline produced better outcomes for reduction of headache days and disability than medication alone.
2017: Powers and Andrew Hershey, MD, PhD, Director, Division of Neurology at Cincinnati Children’s published findings from the Childhood and Adolescent Migraine Prevention (CHAMP) study in The New England Journal of Medicine that reported no clear statistical benefit to the medications over placebo.
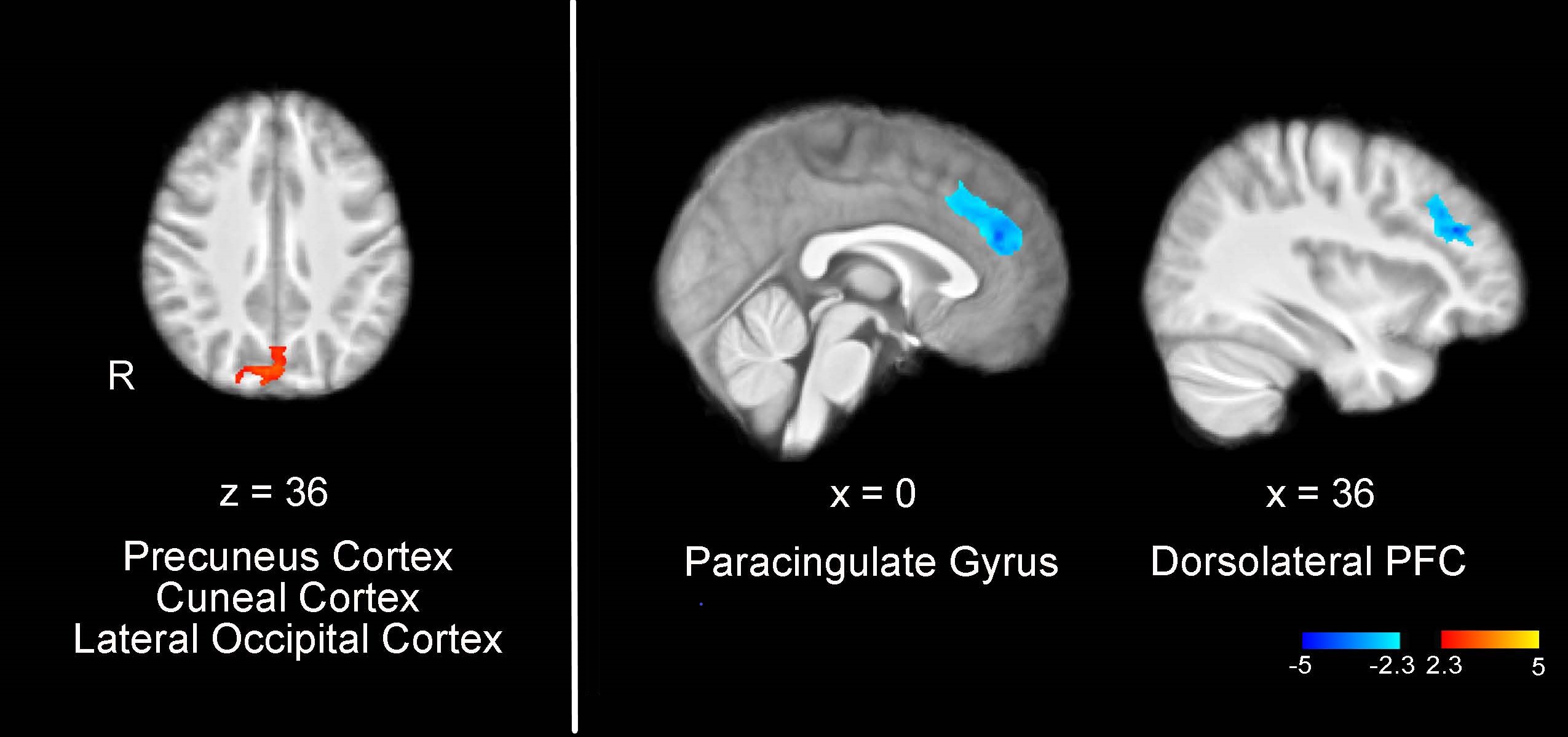
2020: Powers and colleagues published a study in Headache demonstrating that CBT produces measurable changes in brain function, including increased connectivity between the amygdala and frontal regions as well as a reduction in headache frequency.
2021: Powers, Hershey and experts at the University of Iowa published a three-year follow-up study in JAMA Network Open reporting that CHAMP participants maintained the improvements they gained from treatments received even after they stopped taking the medications or the placebo. Co-authors theorized then that simply participating in the CHAMP study allowed the youths to gain deeper understanding of their migraine disease and learn how to adjust their behaviors and healthy habits to manage the headaches.
Meanwhile, the COVID-19 pandemic caused a dramatic increase in the use of telehealth services in pediatric medicine, especially in mental health and behavioral care. That shift has made it necessary to specifically look at telehealth-provided care for migraine as well, Powers says.
With these shifts, more data is needed to determine if medication has an additional benefit beyond CBT alone—especially when provided via telehealth. By involving young people recruited at 15 centers across the country, the research team hopes to assemble enough participants to reach conclusive findings.
Recruitment is slated to begin in May 2023. The participating centers are located in New York, California, Kentucky, Colorado, Ohio, Pennsylvania, West Virginia, Delaware, Alabama, Georgia, Virginia, Arizona, and Indiana.
This project was selected through a PCORI funding announcement specifically focused on comparing medications and evidence-based nonmedication treatments for migraine. Several medications are available for migraine and there is also growing interest in the use of nonpharmacological therapies.
“This study was selected for PCORI funding for its potential to provide real-world data on the comparative effectiveness of medication and nonpharmacologic treatments for the prevention of migraine among pediatric patients,” said PCORI Executive Director Nakela Cook, MD, MPH. “We look forward to following the study’s progress and working with Cincinnati Children’s to share the results.”
The award to Cincinnati Children’s has been approved pending completion of a business and programmatic review by PCORI staff and issuance of a formal award contract.
PCORI is an independent, nonprofit organization authorized by Congress in 2010. Its mission is to fund research that will provide patients, their caregivers, and clinicians with the evidence-based information needed to make better-informed healthcare decisions. For more information about PCORI’s funding, visit www.pcori.org.
Learn more about the Headache Center at Cincinnati Children’s
Research By